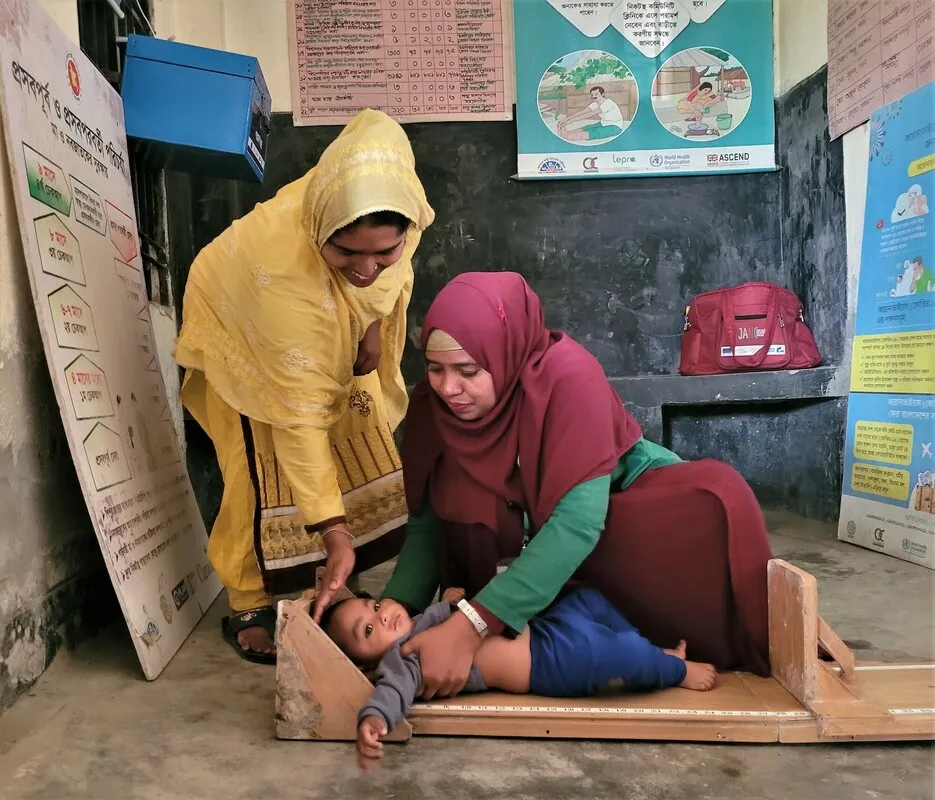
Due to the chronic shortfall in global health workers and increasing health needs, frontline community health workers – 70% of whom are women – face heavy work burdens, resulting in burnout and thereby impacting their work efficiency and effectiveness.
Supporting frontline community health workers is key to achieving global health goals and preparing for the next pandemic. And strong global health systems require equality: equal recognition, support, and fair pay for ALL health workers.
How will we get there?
CARE is committed to working with governments around the world to adequately support, train, and compensate frontline community health workers.